Items filtered by date: May 2018
Plantar Fasciitis
The plantar fascia is a connective tissue in the heel that stretches across the bottom length of your foot. Plantar fasciitis occurs when the connective tissue becomes inflamed, causing heel pain and discomfort during physical activity. Although the condition is completely treatable, traditional methods can take up to a year to start becoming effective.
Plantar fasciitis is caused by a number of everyday activities, so understanding the condition is important for managing and treating it. One of the most common causes of plantar fasciitis is excessive running, especially with improper fitting or non-supportive shoes. Too much exercise can lead to the plantar fascia being overworked and overstretched, which can cause tears in the tissue. Along with improper fitting shoes, pronation, the rolling of the feet inward, is a common cause of plantar fasciitis. If not treated properly, the plantar fascia becomes overstretched and starts to tear, causing inflammation.
Despite the common causes of plantar fasciitis, there are many different treatment options. For less severe cases, conservative home remedies include taking anti-inflammatory drugs to alleviate pain, applying ice packs to the bottom of your foot and heel, slowly stretching and exercising your feet to re-strengthen the tissue, and using orthotic devices are all ways to help manage your plantar fasciitis.
For more severe cases, shockwave therapy has become a common solution for plantar fasciitis. Shockwave therapy can effectively break up the tissue on the bottom of your foot which facilitates healing and regeneration. This fights the chronic pain caused by plantar fasciitis. Even if this doesn’t work, surgery is always a final option. Surgery on the tissue itself can be done to permanently correct the issue and stop the inflammation and pain in your heels.
No matter what the case may be, consulting your podiatrist is the first and best step to recovery. Even the slightest amount of heel pain could be the first stage of plantar fasciitis. Untreated symptoms can lead to the tearing and overstretching of tissue. Because the tearing of tissue can be compounded if it remains ignored, it can evolve into a severe case. The solution is early detection and early treatment. Talk to your podiatrist about the possibilities of plantar fasciitis if you’re experiencing heel pain.
Healing Your Heel Pain
 Plantar fasciitis tends to gradually develop over time and usually only affects one foot. Common symptoms for those with plantar fasciitis are a dull, sharp, or burning pain in the bottom of the foot. This pain tends to start up after prolonged activity due to increased inflammation. People who are overweight are at a greater risk of developing plantar fasciitis because of the increased amount of pressure on the plantar fascia ligaments. Consequently, women who are pregnant also are more likely to develop plantar fasciitis. Other people who are more likely to develop the condition are those with either flat feet, or high arches in their feet. Thankfully, there are some ways to treat pain that stems from plantar fasciitis. One of the most common methods of treatment is icing. In addition, stretching the calves will help alleviate pain in the foot. If you have any questions or concerns regarding plantar fasciitis, a consultation with a podiatrist is advised.
Plantar fasciitis tends to gradually develop over time and usually only affects one foot. Common symptoms for those with plantar fasciitis are a dull, sharp, or burning pain in the bottom of the foot. This pain tends to start up after prolonged activity due to increased inflammation. People who are overweight are at a greater risk of developing plantar fasciitis because of the increased amount of pressure on the plantar fascia ligaments. Consequently, women who are pregnant also are more likely to develop plantar fasciitis. Other people who are more likely to develop the condition are those with either flat feet, or high arches in their feet. Thankfully, there are some ways to treat pain that stems from plantar fasciitis. One of the most common methods of treatment is icing. In addition, stretching the calves will help alleviate pain in the foot. If you have any questions or concerns regarding plantar fasciitis, a consultation with a podiatrist is advised.
Plantar fasciitis is a common foot condition that is often caused by a strain injury. If you are experiencing heel pain or symptoms of plantar fasciitis, contact one of our podiatrists from Carolina Foot & Ankle. Our doctors can provide the care you need to keep you pain-free and on your feet.
What Is Plantar Fasciitis?
Plantar fasciitis is one of the most common causes of heel pain. The plantar fascia is a ligament that connects your heel to the front of your foot. When this ligament becomes inflamed, plantar fasciitis is the result. If you have plantar fasciitis you will have a stabbing pain that usually occurs with your first steps in the morning. As the day progresses and you walk around more, this pain will start to disappear, but it will return after long periods of standing or sitting.
What Causes Plantar Fasciitis?
- Excessive running
- Having high arches in your feet
- Other foot issues such as flat feet
- Pregnancy (due to the sudden weight gain)
- Being on your feet very often
There are some risk factors that may make you more likely to develop plantar fasciitis compared to others. The condition most commonly affects adults between the ages of 40 and 60. It also tends to affect people who are obese because the extra pounds result in extra stress being placed on the plantar fascia.
Prevention
- Take good care of your feet – Wear shoes that have good arch support and heel cushioning.
- Maintain a healthy weight
- If you are a runner, alternate running with other sports that won’t cause heel pain
There are a variety of treatment options available for plantar fasciitis along with the pain that accompanies it. Additionally, physical therapy is a very important component in the treatment process. It is important that you meet with your podiatrist to determine which treatment option is best for you.
If you have any questions, please feel free to contact one of our offices located in Huntersville Office | 16419 Northcross Dr Suite A, Huntersville, NC 28078; Mooresvillle Office | 206 Joe Knox Avenue Suite D, Mooresville, NC 28117; and Mountain Island | 10310 Couloak Drive Suite 200, Charlotte, NC 28216 . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Athlete's Foot
Athlete’s foot is an extremely contagious infection caused by a fungus that results in itching, burning, dry, and flaking feet. The fungus that causes athlete’s foot is known as tinea pedis and thrives in moist, dark areas such as shower floors, gyms, socks and shoes, commons areas, public changing areas, bathrooms, dormitory style houses, locker rooms, and public swimming pools. Athlete’s foot is difficult to treat as well because of the highly contagious and recurrent nature of the fungus.
Tinea is the same fungus that causes ringworm, and is spread by direct contact with an infected body part, contaminated clothing, or by touching other objects and body parts that have been exposed to the fungus. Because the feet are an ideal place for tinea to grow and spread, this is the most commonly affected area. It is, however, known to grow in other places. The term athlete’s foot describes tinea that grows strictly on the feet.
The most commonly infected body parts are the hands, groin, and scalp, as well as the feet. Around 70% of the population suffer from tinea infections at some point in their lives, however not all of these cases are athlete’s foot. Just like any other ailment, some people are more likely to get it than others, such as people with a history of tinea infections or other skin infections, both recurring and non-recurring ones. The extent to which a person experiences regrowth and recurrent tinea infections varies from person to person.
Sometimes people will not even know that they are infected with tinea or that they have athlete’s foot because of a lack of symptoms. However, most experience mild to moderate flaking, itching, redness, and burning. However, some of the more severe symptoms include cracking and bleeding skin, intense itching and burning, pain while walking or standing, and even blistering.
Because of the recurring nature of the tinea fungus and the athlete’s foot it causes, the best way to treat this condition is with prevention. You can take some preventative measures such as wearing flip flops or sandals in locker rooms and public showers to reduce contact with the floor. It also helps to keep clean, dry feet while allowing them to breathe. Using powders to keep your feet dry is a good idea, as well as keeping your feet exposed to light and cool air, to prevent the growth of tinea. If you do happen to get athlete’s foot, opt for using topical medicated creams, ointments or sprays. These treatments help eliminate and prevent it from coming back.
Causes of Athlete’s Foot
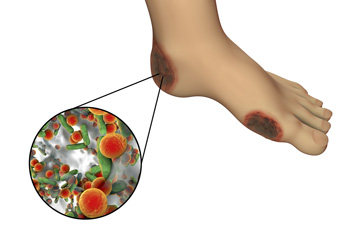 If you experience redness, itchiness, or blisters on the soles of the feet, you may have what is referred to as tinea pedis, or more commonly, athlete’s foot. It is caused by a fungal infection, and is can be extremely contagious. This type of fungus lives and thrives in moist places, and is commonly found in public showers, pools, and surrounding areas. It may affect the area between the toes in addition to the soles of the feet. There are several symptoms of athlete's foot that may be observed, including a rash that may appear, peeling skin on the soles of the feet, or an uncomfortable burning sensation. To prevent this condition from occurring it's suggested to wear appropriate shoes in public places, and to change your socks daily to avoid excessive perspiration between the toes. If you are experiencing chronic or severe athlete’s foot please schedule a consultation with a podiatrist.
If you experience redness, itchiness, or blisters on the soles of the feet, you may have what is referred to as tinea pedis, or more commonly, athlete’s foot. It is caused by a fungal infection, and is can be extremely contagious. This type of fungus lives and thrives in moist places, and is commonly found in public showers, pools, and surrounding areas. It may affect the area between the toes in addition to the soles of the feet. There are several symptoms of athlete's foot that may be observed, including a rash that may appear, peeling skin on the soles of the feet, or an uncomfortable burning sensation. To prevent this condition from occurring it's suggested to wear appropriate shoes in public places, and to change your socks daily to avoid excessive perspiration between the toes. If you are experiencing chronic or severe athlete’s foot please schedule a consultation with a podiatrist.
Athlete’s Foot
Athlete’s foot is often an uncomfortable condition to experience. Thankfully, podiatrists specialize in treating athlete’s foot and offer the best treatment options. If you have any questions about athlete’s foot, consult with one of our podiatrists from Carolina Foot & Ankle. Our doctors will assess your condition and provide you with quality treatment.
What Is Athlete’s Foot?
Tinea pedis, more commonly known as athlete’s foot, is a non-serious and common fungal infection of the foot. Athlete’s foot is contagious and can be contracted by touching someone who has it or infected surfaces. The most common places contaminated by it are public showers, locker rooms, and swimming pools. Once contracted, it grows on feet that are left inside moist, dark, and warm shoes and socks.
Prevention
The most effective ways to prevent athlete’s foot include:
- Thoroughly washing and drying feet
- Avoid going barefoot in locker rooms and public showers
- Using shower shoes in public showers
- Wearing socks that allow the feet to breathe
- Changing socks and shoes frequently if you sweat a lot
Symptoms
Athlete’s foot initially occurs as a rash between the toes. However, if left undiagnosed, it can spread to the sides and bottom of the feet, toenails, and if touched by hand, the hands themselves. Symptoms include:
- Redness
- Burning
- Itching
- Scaly and peeling skin
Diagnosis and Treatment
Diagnosis is quick and easy. Skin samples will be taken and either viewed under a microscope or sent to a lab for testing. Sometimes, a podiatrist can diagnose it based on simply looking at it. Once confirmed, treatment options include oral and topical antifungal medications.
If you have any questions, please feel free to contact one of our offices located in Huntersville Office | 16419 Northcross Dr Suite A, Huntersville, NC 28078; Mooresvillle Office | 206 Joe Knox Avenue Suite D, Mooresville, NC 28117; and Mountain Island | 10310 Couloak Drive Suite 200, Charlotte, NC 28216 . We offer the newest diagnostic and treatment technologies for all your foot care needs.
How Obesity Affects Your Feet
Gaining weight can happen suddenly and at any time. Usually you won’t notice the extra weight until your feet start hurting at the end of the day. This happens as your feet begin adjusting to carrying more weight. Foot swelling and pain are two of the biggest side effects of having gained weight.
Many foot-related problems can occur even after just putting on a few pounds. This includes the body ‘compensating’ by changing the way it moves. You may find yourself putting extra weight on the wrong parts of your feet and even leaning forward a bit. Your feet were designed to carry a healthy, normal body weight. Extra weight places undue stress on them.
Being overweight often causes the development of Type-2 diabetes, causing leg and foot pain. Older people who do not attempt to control their condition can even lose sensation and feeling in their legs and feet. This can lead to the development of small sores that can lead to serious infection.
Extra stress placed on the joints, tendons and muscles in the feet as a result of extra body weight may also cause heel spurs, or plantar fasciitis. Plantar fasciitis is an inflammation of the foot tissue, causing stiffness and pain when walking and climbing stairs. This can usually be relieved by foot stretches and custom made orthotic shoe-inserts.
Problems in the feet triggered by obesity can be treated by paying special attention to footwear. Proper support shoes that allow for good circulation, especially in the arch and ankle, are vital. A podiatrist can help you find what sort of shoe is most suitable for your feet. They can also measure you for special orthotics if necessary.
It could also be high time to start losing weight in order to treat and prevent diabetes as well as other life threatening diseases. Some methods include yoga and water aerobics, which benefit your entire body without placing stress on your feet. Don’t risk losing your feet by losing interest in them. Take care of your feet and your body, as they deserve the very best.
Foot Conditions That May Develop From Obesity
 Recent research has shown a connection between foot pain and being obese. Foot ailments that may develop as a result of obesity include flat feet, arthritis, diabetes and general heel pain. Obesity may alter the general structure of the foot as a result of the heels and ankles enduring additional pressure caused by excess weight. Exercising may become difficult due to an increase in weight, and this may hinder one's ability to shed the excess pounds. Your feet will benefit if you choose to wear wide and supportive shoes, although there may be a limited selection of larger sizes necessary to accommodate them. Implementing a daily exercise routine and maintaining a healthy lifestyle may aid in combating obesity. This can typically be achieved by slowly beginning to properly stretch and exercise the feet. Please consider scheduling a consultation with a podiatrist for a recommended exercise program that may avoid foot pain.
Recent research has shown a connection between foot pain and being obese. Foot ailments that may develop as a result of obesity include flat feet, arthritis, diabetes and general heel pain. Obesity may alter the general structure of the foot as a result of the heels and ankles enduring additional pressure caused by excess weight. Exercising may become difficult due to an increase in weight, and this may hinder one's ability to shed the excess pounds. Your feet will benefit if you choose to wear wide and supportive shoes, although there may be a limited selection of larger sizes necessary to accommodate them. Implementing a daily exercise routine and maintaining a healthy lifestyle may aid in combating obesity. This can typically be achieved by slowly beginning to properly stretch and exercise the feet. Please consider scheduling a consultation with a podiatrist for a recommended exercise program that may avoid foot pain.
The more you weigh, the harder your feet must work to support your body. If you’re an obese individual and are concerned about your feet, contact one of our podiatrists from Carolina Foot & Ankle. Our doctors can provide the care you need to keep you pain-free and on your feet.
Obesity and Your Feet
People who are overweight are putting more pressure on their ankles, knees, and hips as well as their feet. This unfortunately can lead to variety of different issues.
Problems & Complications Stemming from Obesity
- When the body is overweight, it tries to compensate by changing the way that it moves. An obese person may lean forward and put extra weight on the wrong part of the foot. This puts unnecessary stress on the feet.
- Obese people are also more likely to develop type II diabetes which is a condition that causes a lot of foot problems. People with diabetes often don’t feel the cuts and sores that they may have on their feet, which can lead to more complicated and severe issues.
- Plantar fasciitis is another foot condition that can be caused by obesity. Plantar fasciitis is an inflammation of the tissue along the bottom of the foot, which causes pain and stiffness while walking and climbing stairs.
If you have any questions, please feel free to contact one of our offices located in Huntersville Office | 16419 Northcross Dr Suite A, Huntersville, NC 28078; Mooresvillle Office | 206 Joe Knox Avenue Suite D, Mooresville, NC 28117; and Mountain Island | 10310 Couloak Drive Suite 200, Charlotte, NC 28216 . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Bunions
A bunion is an enlargement of the base joint of the toe that connects to the foot, often formed from a bony growth or a patch of swollen tissues. It is caused by the inward shifting of the bones in the big toe, toward the other toes of the foot. This shift can cause a serious amount of pain and discomfort. The area around the big toe can become inflamed, red, and painful.
Bunions are most commonly formed in people who are already genetically predisposed to them or other kinds of bone displacements. Existing bunions can be worsened by wearing improperly fitting shoes. Trying to cram your feet into high heels or running or walking in a way that causes too much stress on the feet can exacerbate bunion development. High heels not only push the big toe inward, but shift one's body weight and center of gravity towards the edge of the feet and toes, expediting bone displacement.
A podiatrist knowledgeable in foot structure and biomechanics will be able to quickly diagnose bunions. Bunions must be distinguished from gout or arthritic conditions, so blood tests may be necessary. The podiatrist may order a radiological exam to provide an image of the bone structure. If the x-ray demonstrates an enlargement of the joint near the base of the toe and a shifting toward the smaller toes, this is indicative of a bunion.
Wearing wider shoes can reduce pressure on the bunion and minimize pain, and high heeled shoes should be eliminated for a period of time. This may be enough to eliminate the pain associated with bunions; however, if pain persists, anti-inflammatory drugs may be prescribed. Severe pain may require an injection of steroids near the bunion. Orthotics for shoes may be prescribed which, by altering the pressure on the foot, can be helpful in reducing pain. These do not correct the problem; but by eliminating the pain, they can provide relief.
For cases that do not respond to these methods of treatment, surgery can be done to reposition the toe. A surgeon may do this by taking out a section of bone or by rearranging the ligaments and tendons in the toe to help keep it properly aligned. It may be necessary even after surgery to wear more comfortable shoes that avoid placing pressure on the toe, as the big toe may move back to its former orientation toward the smaller toes.
How to Treat a Bunion
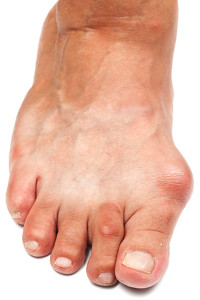 Bunions are typically the result of a bone deformity that affects the toes. The big toe typically leans toward the second toe, and this may cause a bump to form on the bottom of the big toe. Fluid may develop in the surrounding joint, in addition to the skin becoming thickened. This is often a painful condition, and as a result other ailments such as arthritis may develop. Research has shown that it’s beneficial to wear proper shoes that can accommodate the bunion and possibly diminish the pain and discomfort. Relief options may include using adequate padding over the bunion for protection, and wearing shoes that can adjust to the width of your foot. For bunions that have become extremely painful and unmanageable, surgery may be an option to consider. It’s suggested to schedule a consultation with a podiatrist to learn about the best treatment options for you.
Bunions are typically the result of a bone deformity that affects the toes. The big toe typically leans toward the second toe, and this may cause a bump to form on the bottom of the big toe. Fluid may develop in the surrounding joint, in addition to the skin becoming thickened. This is often a painful condition, and as a result other ailments such as arthritis may develop. Research has shown that it’s beneficial to wear proper shoes that can accommodate the bunion and possibly diminish the pain and discomfort. Relief options may include using adequate padding over the bunion for protection, and wearing shoes that can adjust to the width of your foot. For bunions that have become extremely painful and unmanageable, surgery may be an option to consider. It’s suggested to schedule a consultation with a podiatrist to learn about the best treatment options for you.
If you are suffering from bunion pain, contact one of our podiatrists of Carolina Foot & Ankle. Our doctors can provide the care you need to keep you pain-free and on your feet.
What Is a Bunion?
Bunions are painful bony bumps that usually develop on the inside of the foot at the joint of the big toe. As the deformity increases over time, it may become painful to walk and wear shoes. Women are more likely to exacerbate existing bunions since they often wear tight, narrow shoes that shift their toes together. Bunion pain can be relieved by wearing wider shoes with enough room for the toes.
Causes
- Genetics – some people inherit feet that are more prone to bunion development
- Inflammatory Conditions - rheumatoid arthritis and polio may cause bunion development
Symptoms
- Redness and inflammation
- Pain and tenderness
- Callus or corns on the bump
- Restricted motion in the big toe
In order to diagnose your bunion, your podiatrist may ask about your medical history, symptoms, and general health. Your doctor might also order an x-ray to take a closer look at your feet. Nonsurgical treatment options include orthotics, padding, icing, changes in footwear, and medication. If nonsurgical treatments don’t alleviate your bunion pain, surgery may be necessary.
If you have any questions, please feel free to contact one of our offices located in Huntersville Office | 16419 Northcross Dr Suite A, Huntersville, NC 28078; Mooresvillle Office | 206 Joe Knox Avenue Suite D, Mooresville, NC 28117; and Mountain Island | 10310 Couloak Drive Suite 200, Charlotte, NC 28216 . We offer the newest diagnostic and treatment technologies for all your foot care needs.
