Causes and Implications of Flat Feet
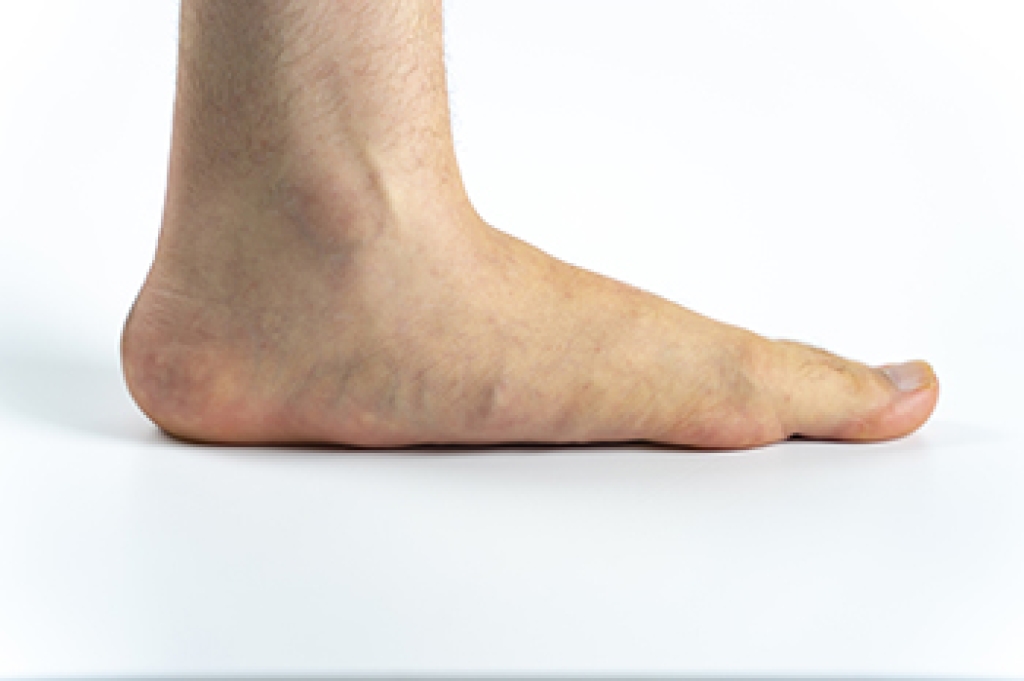
Pes planus, commonly known as flat feet, occurs when the medial longitudinal arch of the foot collapses. This results in the entire sole making contact with the ground, which leads to a flat appearance. Various factors contribute to the development of pes planus. Genetic predisposition plays a significant role, as some individuals inherit a tendency for weak arches. Additionally, obesity places excess strain on the feet, weakening the arch over time. Other causes include injuries or conditions that damage the tendons supporting the arch, such as posterior tibial tendon dysfunction. Chronic conditions like diabetes and rheumatoid arthritis can also contribute to the loss of the arch. If you have flat feet, it is suggested that you are under the care of a podiatrist who can offer you comfort options help you to manage this condition.
Flatfoot is a condition many people suffer from. If you have flat feet, contact one of our podiatrists from Carolina Foot & Ankle. Our doctors will treat your foot and ankle needs.
What Are Flat Feet?
Flatfoot is a condition in which the arch of the foot is depressed and the sole of the foot is almost completely in contact with the ground. About 20-30% of the population generally has flat feet because their arches never formed during growth.
Conditions & Problems:
Having flat feet makes it difficult to run or walk because of the stress placed on the ankles.
Alignment – The general alignment of your legs can be disrupted, because the ankles move inward which can cause major discomfort.
Knees – If you have complications with your knees, flat feet can be a contributor to arthritis in that area.
Symptoms
- Pain around the heel or arch area
- Trouble standing on the tip toe
- Swelling around the inside of the ankle
- Flat look to one or both feet
- Having your shoes feel uneven when worn
Treatment
If you are experiencing pain and stress on the foot you may weaken the posterior tibial tendon, which runs around the inside of the ankle.
If you have any questions please feel free to contact one of our offices located in Huntersville Office | 16419 Northcross Dr Suite A, Huntersville, NC 28078; Mooresvillle Office | 206 Joe Knox Avenue Suite D, Mooresville, NC 28117; and Mountain Island | 10310 Couloak Drive Suite 200, Charlotte, NC 28216 . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
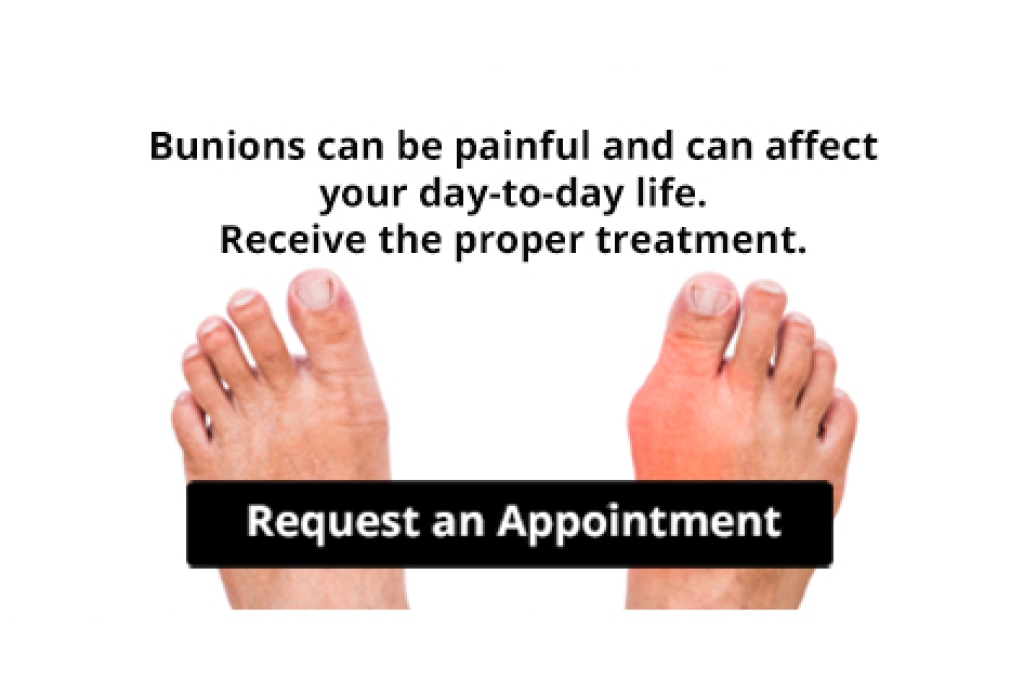
Non-Surgical Treatment for Bunions
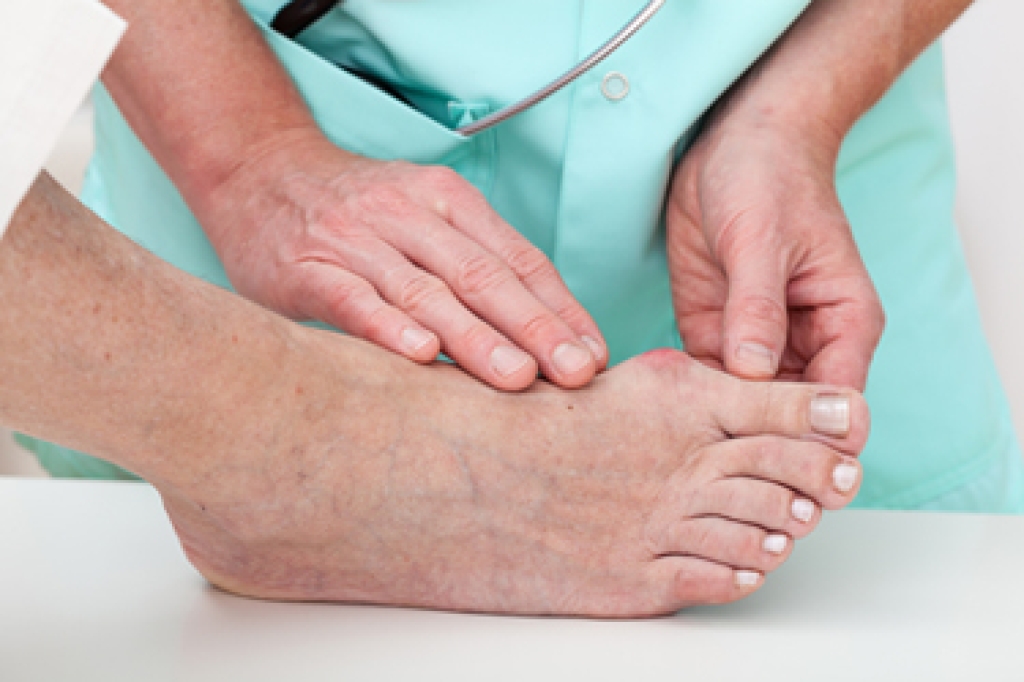
Bunions, a bony bump at the base of your big toe, can result from a misalignment of bones and tissues that pushes the toe inward. While surgery is the only way to completely remove a bunion, nonsurgical bunion treatments can effectively manage symptoms and slow progression. Wearing shoes with a wide toe box and low heels can reduce pressure on the bunion. Custom orthotics can help with proper foot alignment. Toe spacers and splints can also relieve discomfort by preventing further misalignment, although they will not permanently correct the bone structure. Stretching exercises may increase flexibility and ease pain, but they will not reverse the bunion itself. If your bunion is causing discomfort, consulting a podiatrist early can lead to treatment options that delay or prevent further complications. If you have pain caused by a bunion, it is suggested that you schedule an appointment with a podiatrist for guidance.
If you are suffering from bunion pain, contact one of our podiatrists of Carolina Foot & Ankle. Our doctors can provide the care you need to keep you pain-free and on your feet.
What Is a Bunion?
Bunions are painful bony bumps that usually develop on the inside of the foot at the joint of the big toe. As the deformity increases over time, it may become painful to walk and wear shoes. Women are more likely to exacerbate existing bunions since they often wear tight, narrow shoes that shift their toes together. Bunion pain can be relieved by wearing wider shoes with enough room for the toes.
Causes
- Genetics – some people inherit feet that are more prone to bunion development
- Inflammatory Conditions - rheumatoid arthritis and polio may cause bunion development
Symptoms
- Redness and inflammation
- Pain and tenderness
- Callus or corns on the bump
- Restricted motion in the big toe
In order to diagnose your bunion, your podiatrist may ask about your medical history, symptoms, and general health. Your doctor might also order an x-ray to take a closer look at your feet. Nonsurgical treatment options include orthotics, padding, icing, changes in footwear, and medication. If nonsurgical treatments don’t alleviate your bunion pain, surgery may be necessary.
If you have any questions, please feel free to contact one of our offices located in Huntersville Office | 16419 Northcross Dr Suite A, Huntersville, NC 28078; Mooresvillle Office | 206 Joe Knox Avenue Suite D, Mooresville, NC 28117; and Mountain Island | 10310 Couloak Drive Suite 200, Charlotte, NC 28216 . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Understanding Cuboid Syndrome in Athletes
Cuboid syndrome is a common but often overlooked cause of lateral foot pain in athletes, particularly in sports involving running, jumping, and sudden direction changes. It occurs when the cuboid bone, located on the outer side of the foot, becomes partially dislocated or misaligned. Athletes may experience sharp pain, swelling, and difficulty bearing weight. Diagnosis involves a physical examination, including palpation of the cuboid area, range of motion tests, and sometimes imaging like X-rays to rule out fractures. Treatment typically starts with rest. A podiatrist may try to realign the cuboid bone with manual manipulation. They may also use taping or orthotics to support the foot and prevent recurrence. If you participate in sports and have pain on the side of your foot, it is suggested that you schedule an appointment with a podiatrist for a proper diagnosis and treatment.
Cuboid syndrome, also known as cuboid subluxation, occurs when the joints and ligaments near the cuboid bone in the foot become torn. If you have cuboid syndrome, consult with one of our podiatrists from Carolina Foot & Ankle. Our doctors will assess your condition and provide you with quality foot and ankle treatment.
Cuboid syndrome is a common cause of lateral foot pain, which is pain on the outside of the foot. The condition may happen suddenly due to an ankle sprain, or it may develop slowly overtime from repetitive tension through the bone and surrounding structures.
Causes
The most common causes of cuboid syndrome include:
- Injury – The most common cause of this ailment is an ankle sprain.
- Repetitive Strain – Tension placed through the peroneus longus muscle from repetitive activities such as jumping and running may cause excessive traction on the bone causing it to sublux.
- Altered Foot Biomechanics – Most people suffering from cuboid subluxation have flat feet.
Symptoms
A common symptom of cuboid syndrome is pain along the outside of the foot which can be felt in the ankle and toes. This pain may create walking difficulties and may cause those with the condition to walk with a limp.
Diagnosis
Diagnosis of cuboid syndrome is often difficult, and it is often misdiagnosed. X-rays, MRIs and CT scans often fail to properly show the cuboid subluxation. Although there isn’t a specific test used to diagnose cuboid syndrome, your podiatrist will usually check if pain is felt while pressing firmly on the cuboid bone of your foot.
Treatment
Just as the range of causes varies widely, so do treatments. Some more common treatments are ice therapy, rest, exercise, taping, and orthotics.
If you have any questions, please feel free to contact one of our offices located in Huntersville Office | 16419 Northcross Dr Suite A, Huntersville, NC 28078; Mooresvillle Office | 206 Joe Knox Avenue Suite D, Mooresville, NC 28117; and Mountain Island | 10310 Couloak Drive Suite 200, Charlotte, NC 28216 . We offer the newest diagnostic and treatment technologies for all your foot care needs.
How High Heels Affect the Feet

Wearing high heels can significantly alter foot posture and alignment, leading to various long-term issues. These shoes force the foot into an unnatural position, causing the bones and foot structure to deviate from their proper alignment. As a result, the biomechanics of walking are compromised, affecting overall foot function. High heels cause the foot to slide forward, compressing the forefoot, especially in narrower toe boxes, which often leads to increased foot supination. This abnormal alignment can increase the risk of overuse injuries and conditions like hammertoes and bunions. Over time, these biomechanical changes may lead to chronic pain and instability. A podiatrist can assess the damage and offer solutions to ease pain and prevent further complications. If you are experiencing foot pain from wearing high heels, it is suggested that you schedule an appointment with a podiatrist.
High heels have a history of causing foot and ankle problems. If you have any concerns about your feet or ankles, contact one of our podiatrists from Carolina Foot & Ankle. Our doctors can provide the care you need to keep you pain-free and on your feet.
Effects of High Heels on the Feet
High heels are popular shoes among women because of their many styles and societal appeal. Despite this, high heels can still cause many health problems if worn too frequently.
Which Parts of My Body Will Be Affected by High Heels?
- Ankle Joints
- Achilles Tendon – May shorten and stiffen with prolonged wear
- Balls of the Feet
- Knees – Heels cause the knees to bend constantly, creating stress on them
- Back – They decrease the spine’s ability to absorb shock, which may lead to back pain. The vertebrae of the lower back may compress.
What Kinds of Foot Problems Can Develop from Wearing High Heels?
- Corns
- Calluses
- Hammertoe
- Bunions
- Morton’s Neuroma
- Plantar Fasciitis
How Can I Still Wear High Heels and Maintain Foot Health?
If you want to wear high heeled shoes, make sure that you are not wearing them every day, as this will help prevent long term physical problems. Try wearing thicker heels as opposed to stilettos to distribute weight more evenly across the feet. Always make sure you are wearing the proper shoes for the right occasion, such as sneakers for exercising. If you walk to work, try carrying your heels with you and changing into them once you arrive at work. Adding inserts to your heels can help cushion your feet and absorb shock. Full foot inserts or metatarsal pads are available.
If you have any questions please feel free to contact one of our offices located in Huntersville Office | 16419 Northcross Dr Suite A, Huntersville, NC 28078; Mooresvillle Office | 206 Joe Knox Avenue Suite D, Mooresville, NC 28117; and Mountain Island | 10310 Couloak Drive Suite 200, Charlotte, NC 28216 . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.